Clinical Reasoning podczas dostępu bezpośredniego
Hej ty.
Tak jest!
Mam pewne trudności z dolną częścią pleców i mam nadzieję, że możecie mi podsunąć jakieś myśli i wskazówki jak sobie z tym poradzić.
Mam 45 lat, 1,72 m wzrostu i masę ciała około 72 kg. Pracuję jako kierownik kontroli jakości w laboratorium farmaceutycznym, co oznacza, że siedzę przez połowę dnia i czasami podnoszę pudła o wadze od 4,5 do 9 kg.
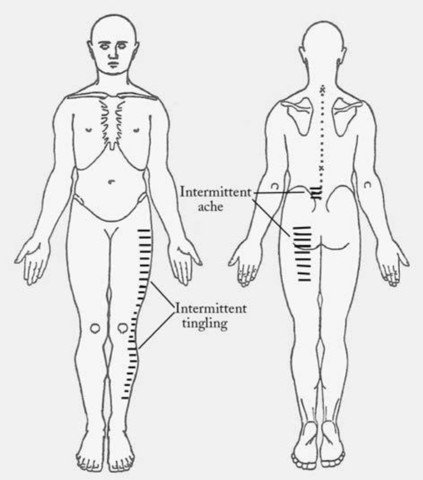
Zarysowałem już dla Was obraz moich objawów. Ból zaczyna się w dolnej części pleców po lewej stronie i rozciąga się na tylną część uda. Ten ból nie występuje stale, zależy od tego co robię. To samo dotyczy mrowienia na bocznej przedniej stronie mojej nogi. Czasem jest ono większe, a czasem mniejsze. Ale to też zależy od tego co robię i przychodzi i odchodzi równolegle z bólem w plecach i nodze.
Hej tam, jestem twoim wewnętrznym głosem klinicznego rozumowania. Właśnie otrzymałem kilka informacji i musimy o nich porozmawiać. Czy uważasz, że problem pacjenta jest bardziej mechaniczny czy niemechaniczny? Ile źródeł dla symptomów spodziewasz się? Czy są jakieś środki ostrożności, na które musimy uważać?
Działania , które zwiększają moje symptomy to leżenie supinujące, kaszel i kichanie, przedłużone chodzenie i siedzenie dłużej niż godzina. Używanie poduszki cieplnej na dolną część pleców i branie 200 mg Ibuprofenu jak co 4 godziny sprawia, że czuję się lepiej.
Rano nie odczuwam dużego bólu, nasila się on wieczorem lub gdy próbuję zasnąć. Czasem też budzę się z powodu bólu, ale gdy znajdę wygodną pozycję, mogę szybko ponownie zasnąć.
Mam już te objawy od kilku miesięcy, ale nie pamiętam żadnego zdarzenia, które tłumaczyłoby ich początek. Właśnie mrowienie zaczęło się jak tydzień temu. Miałem już w przeszłości bóle dolnej części pleców, ale nigdy mnie nie ograniczały i nigdy nie miałem objawów w udzie.
Oprócz Ibuprofenu nie biorę żadnych innych leków. Nie mam nadciśnienia, cukrzycy, wcześniejszej historii raka ani utraty wagi, funkcja pęcherza i miski jest normalna i nie mam żadnych innych obaw dotyczących ogólnego stanu zdrowia. Nie palę i nie brałem sterydów ani leków przeciwzakrzepowych w przeszłości. Jest Pan pierwszą osobą, z którą rozmawiam o moim problemie, więc nie mam żadnych nagrań z poprzednich badań.
Hej, znowu ja. Zastanówmy się nad tym. Co z Twoimi wcześniejszymi przemyśleniami (mechaniczne/nie mechaniczne, źródła, środki ostrożności)? Czy się zmieniły?
Czy objawy są związane z określonym kierunkiem ruchu? Który obszar zbadałbyś dalej? Co spodziewałbyś się znaleźć podczas badania fizycznego?
Czy rozpoznaje pan wzór kliniczny?
To są wyniki mojego pierwszego badania fizycznego (podsumowanie):
Chód lekko antalgiczny (próba uniknięcia bólu) podczas obciążania lewej kończyny dolnej.
Aktywne ruchy
- Rozciąganie umiarkowanie zmniejszone, odtwarzanie bólu dolnej części pleców *.
- Zgięcie niepokojące
- LatFlex lewy lekko obniżony, odtworzenie bólu dolnej części pleców i ud *.
- LatFlex prawy niepodejrzany
W badaniu neurologicznym stwierdzono osłabienie mięśni zginaczy stawu biodrowego lewego i prostowników stawu kolanowego. Odruchy z Achillesa i rzepki były obustronnie prawidłowe.
Ruchy pasywne
- Gibkość bioder, rotacja wewnętrzna i zewnętrzna była obustronnie podobna, bez zmian w objawach.
- Przywiedzenie biodra w zgięciu 90° - o 20° mniejsze w porównaniu do strony prawej, odtworzyło objawy tylnej części uda *.
- Uniesienie prostej nogi na prawą stronę 60°, napięcie w mięśniach prostowników.
- Proste uniesienie lewej nogi o 45°, nasilony ból tylnej części uda lewego *.
Czy wyniki badań pokrywają się z Twoimi wcześniejszymi przemyśleniami? Co jeszcze byś zbadał?
To było moje leczenie:
1st Sesja:
- Ocena jak wyżej
- Leczenie:
- Ogólna technika oscylacji rotacyjnej odcinka lędźwiowego w leżeniu bocznym na prawym boku przez 5 minut (ponowna ocena bez zmian)
- Praca domowa: podobna do techniki leczenia jak automobilizacja co 2 do 3 godzin
- Edukacja w zakresie odpowiednich pozycji podczas snu i siedzenia
2nd Sesja (1 tydzień później)
- Ogólnie bez zmian
- Nieznaczne, przejściowe zmniejszenie bólu po wykonaniu ćwiczenia
- Ponowna ocena bez zmian
- Dodatkowa ocena:
- Central PA C5 zmniejszona ruchomość (w porównaniu do innych poziomów kręgosłupa), odtwarzanie bólu pleców, bólu tylnej części uda i mrowienia przednio-bocznego *.
- Wyciągnięcie biodra w prawo 15°, bez objawów
- Hip Ext left 10°, odtworzenie bólu pleców, bólu tylnej części uda i mrowienia przednio-bocznego *.
- Zmniejszona siła przywodzicieli lewego biodra *.
- Negatywny wynik testu zgięcia kolanowego obustronnie
- Leczenie:
- Jak w 1.st Sesja
- Rozciąganie bioder, aby zająć się odkryciami tam
Kolejne sesje:
- Leczenie odbywało się raz w tygodniu i składało się z interwencji wymienionych w "2nd sesja"
- Ogólnie rzecz biorąc, objawy uległy pogorszeniu
- Zmniejszona tolerancja na siedzenie
- Objawy stały się bardziej stałe
- Chód stał się bardziej antalgiczny, pacjent musiał używać laski jednopunktowej
- Ponowna ocena nie zmieniła się
Od pierwszej sesji minęło 29 dni. Zamiast poprawy, objawy pacjenta pogorszyły się. Dlaczego tak mogło być? Czy pasuje to do naszej dalszej hipotezy? Co powinniśmy zmienić, aby poprawić stan pacjenta?
Hej wszystkim, teraz tym razem jego Sebastian z IMTA ;)
Opisany powyżej pacjent to opis przypadku, który został opublikowany w JOSPT w 2005 roku (Ross i Bayer, 2005). Myślę, że to może być typowy pacjent w Twojej klinice: ból w dolnej części pleców z objawami promieniowania (w tym przypadku ból i mrowienie). Może być prowokowany i łagodzony przy pewnych ruchach i długotrwałych pozycjach. W badaniu fizycznym pojawiły się pewne punkty, które nie były dla mnie w pełni jasne jak:
- nie wspomniano o rotacji lędźwiowej
- co mieli na myśli z osłabieniem w badaniu neurologicznym ("normalne" osłabienie mięśni czy zmniejszone odbicie?).
- brak ruchu uczulającego podczas uniesienia prostej nogi, a więc brak jednoznacznej informacji o potencjalnym źródle nocyceptywnym
Ale ogólnie rzecz biorąc, wyniki badań wskazują na dość mechaniczny problem nocyceptywny (przypuszczalnie z dolnego odcinka lędźwiowego kręgosłupa) z dodatkowym wejściem neurogennym.
Nawet ból nocny reaguje dość mechanicznie, ponieważ uzyskał ulgę po przewróceniu się na drugi bok, a około 58 % pacjentów z bólem dolnego odcinka kręgosłupa budzi się w nocy, nie wykazując podstawowej poważnej patologii (Premkumar et al., 2018).
Jednak po 4 tygodniach interwencji musimy ponownie ocenić nasze wyniki:
- Ból nocny
- Nasilający się ból (konieczność chodzenia o lasce) bez wyraźnej przyczyny
- Nasilenie objawów neurologicznych
- Brak odpowiedzi na leczenie
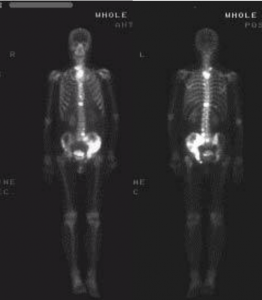
Trochę skracając: u pacjenta ostatecznie zdiagnozowano raka drobnokomórkowego płuca z licznymi obszarami przerzutów kostnych (w kręgosłupie, kości krzyżowej i lewej miednicy/biodrze).
Omówiłem ten przypadek z kilkoma przyjaciółmi, którzy pracują w scenariuszach bezpośredniego dostępu jako fizykoterapeuci. Potwierdzili oni, że czasami czas, ponowna ocena i bieżące rozumowanie kliniczne są najważniejszymi narzędziami do identyfikacji niektórych poważnych mechanizmów patologicznych.
Po ponownym przeczytaniu tej sprawy miałem też kilka take away'ów:
- Odtwarzanie objawów (czynne i bierne) oraz krótkotrwała ulga nie wykluczają poważnej patologii (patrz także opis przypadku Mabry i in., 2014)
- Zmniejszanie bólu poprzez obracanie się w łóżku też nie jest
- Dokonaj ponownej oceny
- Każdy z nas ma dostęp bezpośredni (przyjaciel lub członek rodziny prosi o poradę, pacjent ma zmianę objawów w trakcie oczekiwania na pierwszą wizytę, pacjent skierowany np. z bólem szyi prosi o poradę dotyczącą dolnej części pleców)
Więc teraz nie należy panikować i odsyłać każdego pacjenta do lekarza ;) Najważniejszym pytaniem podczas naszego procesu rozumowania klinicznego powinno być: czy cechy (nadal) pasują?
Dzięki za przeczytanie,
Sebastian
#directaccess #redflag #reflagscreening #lowbackpain #specificpain #maitland #imta #sebsebsen #löscher
Mabry, L.M., Ross, M.D., Tonarelli, J.M., 2014. Metastatic cancer mimicking mechanical low back pain: a case report. J. Man. Manip. Ther. 22, 162-169. https://doi.org/10.1179/2042618613Y.0000000056
Premkumar, A., Godfrey, W., Gottschalk, M.B., Boden, S.D., 2018. Red Flags for Low Back Pain Are Not Always Really Red: A Prospective Evaluation of the Clinical Utility of Commonly Used Screening Questions for Low Back Pain. J. Bone Jt. Surg. 100, 368-374. https://doi.org/10.2106/JBJS.17.00134
Ross, M.D., Bayer, E., 2005. Cancer as a Cause of Low Back Pain in a Patient Seen in a Direct Access Physical Therapy Setting. J Orthop Sports Phys Ther 35, 9.




Uwagi