Est-ce que "étirer" un nerf et "mettre en tension" celui-ci est une terminologie appropriée dans l'enseignement de la thérapie manuelle et dans la pratique quotidienne ?
Avant que vous ne commenciez à lire ce blog, il convient de préciser qu'il se limite à la biomécanique des nerfs périphériques. J'espère qu'il vous donnera quelques idées intéressantes pour l'éducation et le travail clinique.
L'enseignement de l'évaluation du système nerveux périphérique dans les douleurs et les troubles musculo-squelettiques est une partie importante des cours de l'AMTI. Au cours de la dernière décennie, d'autres concepts musculo-squelettiques en Europe ont suivi l'exemple de l'AMTI. Une partie importante de l'évaluation des nerfs consiste à évaluer la mécanosensibilité par des manœuvres standardisées comme le test neurodynamique des membres supérieurs (ULNT), l'élévation de la jambe droite (SLR), le test de l'affaissement et de la flexion du genou couché (PKB). Si l'on se réfère aux programmes d'études, à l'expérience clinique et à la littérature, les professeurs de thérapie manuelle forment leurs étudiants, dans la plupart des cas, sur la base des prémisses suivantes ;
la langue qui est couramment utilisée pendant les cours et la pratique
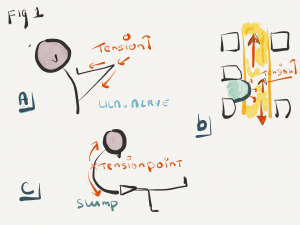
- Les nerfs bougent mais augmentent en tension spéciale s'il y a un "pré-étirement" dans une position neurodynamique standardisée (Fig1.a).
- Les interfaces mécaniques altérées (anormales) réduisent le mouvement des nerfs et augmentent leur "tension" (fig. 1b).
- Les "tendeurs" comme manœuvre de traitement étirent le nerf.
- Les points de tension sont des zones où le nerf s'adapte davantage à la "tension" (fig. 1c).
- La gamme de résistance (de la première résistance R1 jusqu'à la limite de résistance -R2) pendant un test neurodynamique est causée par l'augmentation de la "tension" nerveuse.
Fig1 Exemples de dessins utilisés pour expliquer la neurodynamique pendant l'enseignement et dans la clinique.
1a. Tension ulnaire sur le condyle médial en position neurodynamique extrême du nerf ulnaire
1b. Interface mécanique anormale ; le disque bombé entre en contact avec la moelle épinière pendant le mouvement.
1c Point de tension classique pendant la position d'affaissement
En relation avec ces connaissances, les cliniciens qui ont intégré les connaissances neurodynamiques dans leur pratique peuvent expliquer la mobilisation des nerfs comme un concept plus mécanique où des termes tels que "glissement", "tension" et "étirement" des nerfs sont régulièrement utilisés.
La littérature permet de conclure que les effets biomécaniques, tels que le mouvement, le stress et la tension des tests neurodynamiques et des mouvements des membres, n'ont pas été déterminés de manière systématique, en particulier les effets de la dynamique nerveuse au cours des plages plus terminales des tests neurodynamiques et des techniques de traitement. De la physique stress est définie comme une force par unité de surface. Elle apparaît lors d'un test neurodynamique sous la forme suivante tractionLes contraintes de traction sont des contraintes de compression, de compression et de cisaillement (Abrams et al 1998, entre autres). Les contraintes de traction peuvent être parallèles (longitudinales) ou perpendiculaires (transversales) à l'axe longitudinal du nerf (Topp et al 2006). Souche peut être défini comme la déformation relative d'une structure et peut être estimé à partir de la différence mesurée de l'excursion nerveuse à deux points de mesure différents divisée par la distance entre ces points [Vanti et al 2010, entre autres]. Dans le domaine de la thérapie physique, l'"étirement" d'un nerf est expliqué comme un mouvement qui soumet le tissu à une contrainte maximale tolérable dans le but de provoquer un changement dans la flexibilité du tissu (Topp et al 2006, entre autres).
D'un point de vue factuel, les enseignants et les cliniciens en thérapie manuelle doivent refléter ce qui se passe sur le plan biomécanique avec un nerf périphérique lors de l'augmentation de la résistance et des changements de sensibilité mécanique au cours d'un test ou d'un traitement. La raison en est d'informer les étudiants et les patients de manière plus appropriée et de faciliter les idées pour de nouvelles approches ou modalités de traitement.
Des études réalisées sur des cadavres humains confirment l'hypothèse selon laquelle différentes manœuvres de tests neurodynamiques induisent une augmentation significative de la tension nerveuse (Zoech et al 1991). De plus, les tests s'accompagnent d'une excursion et d'une tension nerveuse longitudinale (Kwan et al 1992). Cependant, on peut se demander si l'on peut transférer les preuves de stress et de tension nerveuse de ce cadre scientifique à des humains vivants. Récemment, une revue systématique de Silva et al. (2014) a examiné les preuves de l'excursion nerveuse longitudinale in vivo pendant différents mouvements articulaires. Les auteurs ont conclu que les articulations pourraient induire un glissement des nerfs plutôt qu'une augmentation de la contrainte (Silva et al 2014).
Une revue systématique publiée par Szikszay et al (2017) sur le comportement mécanique du système nerveux périphérique sous allongement et tension in vivo soutient que ' "étirement" et "tension" pourraient ne pas être la terminologie appropriée. Cette revue a inclus 22 Études et a constaté que pendant le mouvement des nerfs périphériques in vivo, des changements biomécaniques complexes se produisent dans les nerfs périphériques. Ceux-ci consistent en une excursion longitudinale et transversale du nerf et en des changements de diamètre plutôt qu'en un allongement anatomique (incluant l'axone et le tissu conjonctif du nerf). L'augmentation de l'activité musculaire adjacente peut soutenir la résistance clinique (R1-R2) plutôt que la tension ou la contrainte du tissu nerveux. Il est conclu que le mouvement des membres induit des effets biomécaniques complexes dont l'allongement du nerf ne joue qu'un rôle mineur.
De ce point de vue, les éducateurs en thérapie manuelle et les cliniciens devraient utiliser les termes "stress" et "tension" avec prudence. Il serait peut-être bon de les remplacer par les mots "mouvement", "adaptation", "changements de diamètre" lorsqu'ils enseignent et informent les médecins et les patients.
Suggestion d'un langage plus approprié
- Le mouvement des nerfs est complexe et est remis en question lors de l'"adaptation" du mouvement pendant une position neurodynamique normalisée accrue.
- Un nerf est mis au défi par une adaptation de la variabilité des mouvements comme le mouvement transversal ou les changements de diamètre des interfaces mécaniques adjacentes (anormales).
- La résistance ressentie lors d'un "tensionneur" est davantage une augmentation de l'activité musculaire autour du nerf qu'une élongation (tissu conjonctif du nerf ou de l'axone).
- Le mécanisme des points de tension n'est pas connu. Il y a probablement une augmentation de la nociception des tissus environnants lors de la mise en charge du nerf plutôt qu'un étirement ou un allongement du tissu nerveux.
- L'étendue de la résistance (R1-R2) pendant un test neurodynamique peut être liée de manière dominante à une protection musculaire accrue plutôt qu'à une charge nerveuse.
ajustement 2
La figure 2 est une suggestion de croquis/dessin qui peut être utilisé pour expliquer la neurodynamique en évitant les mots "étirement" et "tension".
Fig 2a explication classique de la douleur ou de la mécanosensibilité accrue due à un barrage de fibres Ad C pour le tissu conjonctif du nerf dans la corne dorsale par un stress accru, une tension du nerf.
Fig 2b Explication de la douleur/ mécanosensibilité de l'augmentation de l'activité musculaire par laquelle la tension/douleur est associée à une augmentation du barrage de fibres Ad et C du muscle plus que du nerf qui s'adapte toujours au mouvement.
Bonne chance :-)
Harry von Piekartz
Littérature
Abrams RA, Butler JM, Bodine-Fowler S, Botte MJ. Tensile properties of the neurorrhaphy site in the rat sciatic nerve. J Hand Surg Am 1998 ; 23(3) : 465-70
Kwan MK, Wall EJ, Massie J, Garfin SR. Déformation, stress et étirement des expériences sur les nerfs périphériques chez le lapin in vitro et in vivo. Acta Orthop Scand 1992 ; 63(3) : 267-72
Silva A, Manso A, Andrade R, Domingues V, Brandão MP, Silva AG. Quantitative in vivo l'excursion et la déformation du nerf longitudinal en réponse à un mouvement articulaire : Une revue systématique de la liter- ature. Clin Biomech (Bristol, Avon) 2014 ; 29(8) : 839- 47. doi : 10.1016/j.clinbiomech.2014.07.006.
SzikszayT,Hall T,von Piekartz H. Effets in vivo du mouvement des membres sur l'étirement, la contrainte et la tension nerveuse : Une revue systématique , Journal of Back and Musculoskeletal Rehabilitation -1 (2017) 1-16 DOI 10.3233/BMR-169720.
Topp KS, Boyd BS. Structure et biomécanique des nerfs périphériques : Nerve responses to physical stresses and implications for physical therapist practice. Phys Ther 2006 ; 86(1) : 92-109
Vanti C, Bonfiglioli R, Calabrese M, Marinelli F, Guccione A, Violante FS, Pillastrini P. Upper limb neurodynamic test 1 and symptoms reproduction in carpal tunnel syndrome. A validity study. Manual Therapy 2011 ; 16(3) : 258-263. doi : 10. 1016/j.math.2010.11.003.
Zoech G, Reihsner R, Beer R, Millesi H. Stress et tension dans les nerfs périphériques. Neuro Orthop 1991 ; 73-82.




Commentaires