Are we talking about Core stability? Or ist lumbar movement control the appropriate term?
In 2021, I have been lucky to have been selected by the authors of the study “Lumbar movement control in non-specific chronic low back pain: Evaluation of a direction-specific battery of tests using item response theory” (Adelt, et al), to participate in their study as an examiner. This participation gave me the opportunity to update my knowledge and understanding in the area of motor control.
In this blog I would like to share my experience and give you an inside in this relevant topic for NMSK therapists.Background of the study
LBP continues to be a major burden. More than 85% of patients suffer non-specific LBP with multifactorial causes, amongst which poor lumbar motor control (LMC). Although, to date there is no clear and widely accepted definition of LMC, most sources accept the definition where LMC is seen as the ability to actively control movements in the lumbar spine, while concurrently producing movement elsewhere (Hides et al 2001; Saragiotto et al, 2016). In poor LMC, excessive tissue loading can lead to injuries (Sahrman et al, 2017).
Why item response theory (IRT)?
The study used the so called Item Response Theory the explanation is given by Thomas Schöttker-Königer one of the authors:
If different tests measure the same, you have to summarize the test results. In the case of lumbar movement control, all the tests are named as latent constructs. This means the construct cannot be judged directly via just one test, various tests are necessary.
The tests of LMC are evaluated binary (correct / not correct). This might be one reason, to use the IRT instead of the classical test theory.
One advantage of IRT seems the ability to assess the patient underlying construct (here lumbar movement control). Not all tests of the battery have to be performed, which is often not possible in daily practice. If the difficulty of a test in known, one can determine, with a certain tolerance (uniqueness), how good the patient performs.
The objectives of the study were:
- Is LMC best measured direction-specifically or uni-dimensionally?
- Validation of a test battery measuring LMC
- Quantification of the ability of patients with NSCLBP to actively control movements of the Lumbar Spine
Between April and September 2019, 21 manual therapists of 19 outpatients PT clinics in Germany and Austria recruited a total of 277 patients with NSCLBP.
Specific training for the physiotherapists participating in the study was given by written paper and a lot of video based material with very thorough descriptions of the different test positions.
Prior to physical examination testing for motor control, the following tools were used in the study to assess sense of movement and LBP characteristics:
- Fear Avoidance Beliefs Questionnaire (FABQ): pain related fear
- Fremantle Back Awareness Questionnaire (FreBAQ): impaired perceptual body image
- Numeric rating scales: Pain related disability during daily activities , pain intensity and sense of movement
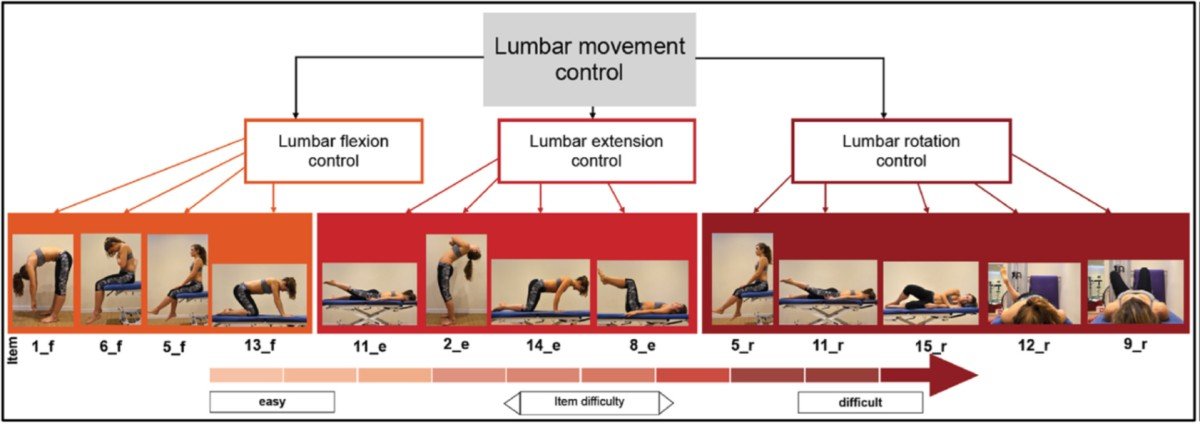
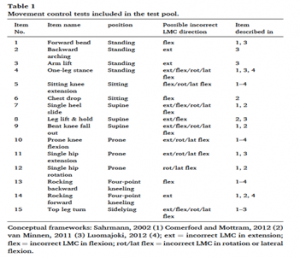
The following 15 tests for LMC were assessed (4 items for extension, 4 for flexion and 5 items for lateral flexion/rotation).
(Pictures and tables used with permission of the authors)
More than 80% of all participants showed at least one incorrect direction of LMC.
15 items are the 15 tests, with different direction and various difficulties. The test battery reveal that flexion control tests are less difficult than extension control tests. Rotation-specific tests are the most difficult ones and showed the highest standard deviation (SD) poorer than average.
For screening purpose a selection of the most sensitive tests to identify poor motor control might be chosen:
| For flexion | “rocking backward in four point kneeling” |  |
| For extension | “leg lift & holding supine” |  |
| For rotation/lateral flexion | “single hip rotation in prone” |  |
Each direction of LMC should be examined separately. This might is the most obvious difference compared to other test procedures.
A test was rated as “incorrect” if movement in the lumbar spine occurred prematurely and/or excessively into the specific direction (extension, flexion ore rotation/lateral flexion) based on the subjective judgement of a trained investigator. Decision on an incorrect test was based on eyeballed estimation. The eyeball estimation about the test outcome was defined by protocol.
Critical aspects
The tester defined the test as correct or incorrect by eyeballed estimation, which might be difficult by less experienced physiotherapists. A control group without lumbar symptoms was missing in the study.
Comparison to other studies
Other authors like Luomajoki et al (2008), postulated a test procedure which differentiates between patients with and without LBP. The patients showed 2.21 incorrect tests compared to 0.75 in the healthy control group. They tested about the same number of participants (210 ) and 12 investigators took part. The tests weren`t split in different movement directions.
This large number of patients represented a good cross section of patient with NSCLBP compared to other studies with less patients, although a large number of investigators could cause a large subjective fail or incorrect decision concerning the test evaluation.
Wattananon et al (2021), published a study on lumbar motor control with only 8 patients and 8 healthy subjects and came to a total different result.
They tested active prone hip rotation, this test was marked as very sensitive in the study of Adelt. Participants with LBP used a lumbopelvic stiffening strategy for postural control to protect painful structures. The mean of this test results contradict the outcome of the study from Adelt. 
In this study, consecutive rotational movement in the back didn`t take place because the patients stiffened their lumbar spine for protection. The study of Adelt et al would rate this outcome as a “correct”. They would estimate patients with NSCLBP rotate their lumbar spine while rotate the hip and would not be able to control this consecutive movement.
Several tests are mentioned in the vast literature on this topic. Finding the most appropriate ones for the patient’s need is key. Interestingly, a paper of Hides et al (2019), offers an overview of different approaches for the management of low back pain patients, without mentioning chronic low back pain patients! Based on experience, lumbar movement control impairments will be seen most in patients with a long history of back pain.
Hides et al (2019) describes: Movement System Impairments; Mechanical Diagnosis and Therapy; Motor Control Training and the Integrated Systems Model. The underlying assumption that the manner in which a person “uses” their body and loads their tissues is related to the development and maintenance of their condition. In my opinion a very interesting article, which needs to be highlighted in an another blog.
Overall summary of that article of Hides: “no evidence supports one treatment approach over another”. “However, the reliable identification of members of subgroups for which there are predictably effective, subgroup-specific treatments begins with the process of identifying standardized treatment for members of that subgroup”. (Hides et al 2019, Saragiotto et al 2017)
Are we sure we want standardized treatments?
Seeing all of us in the process of looking for subgroups and relevant treatment options for patients with LMC and NSCLBP.
Or looking for patients with Core stability problems? Consult Mrs. Klein-Vogelbach`s publications!!!
Literature:
Adelt, E., Schoettker-Koeniger, T., Luedtke, K., Hall, T., Schäfer, A., 2021. Lumbar movement control in non-specific chronic low back pain: Evaluation of a direction-specific battery of tests using item response theory. Muskuloskelettal Science and Practice 55 (2021) 102406
Luomajoki, H., Koll, J., de Bruin, ED., Airaksinen, O., 2008. Movement control tests of the low back; evaluation of the difference between patients with low back pain and healthy controls. BMC Musculoskeletal Disorder. 9, 170-170
Wattananon, P., Siflies S.P., Wang, H.K., 2021. Patients with low back pain use stiffening strategy to compensate for movement control during active prone hip rotation: A cross-sectional study. Journal of Back an Musculoskeletal Rehabilitation-1, 1-10
Hides, J. Donelson, R., Lee, D., Prather, H., Sahrmann, S., Hodges, P,. June 2019. Convergence and Divergence Between Exercise Based Approaches for Management of Low Back Pain That Consider Motor Control. Journal of Orthopaedic & Sports physical therapy, volume 49, number 6
Sahrmann S, et al. Diagnosis and treatment of movement system impairment syndromes. Braz J Phys Ther. 2017 Nov-Dec; 21(6): 391–399Saragiotto Bruno T, Maher Christopher G , Yamato Tiê P , Costa Leonardo O P , Costa Luciola C Menezes , Ostelo Raymond W J G , Macedo Luciana G. Motor control exercise for chronic non-specific low-back pain. Cochrane Database Syst Rev 2016 Jan 8;2016(1)
Saragiotto Bruno T., Maher Chris G., Hancock Mark J., Koes Bart W. Subgrouping Patients With Nonspecific Low Back Pain: Hope or Hype? J Orthop Sports Phys Ther 2017;47(2):44-48.
#lumbar movement control #non specific low back pai#core stability# lumbar exercises




Comments