La cause de la cause... à la recherche de nos points aveugles dans la connaissance et la compréhension des schémas cliniques
Les cliniciens expérimentés utilisent la reconnaissance des formes dans leur raisonnement clinique en s'appuyant sur une base de connaissances étendue pour rechercher des modèles familiers (Feltovich & Barrows, 1984). La reconnaissance des schémas offre un moyen rapide et efficace de formuler une hypothèse qui servira de base à la prise en charge du patient. Cependant, une prise en charge basée uniquement sur la reconnaissance des schémas peut conduire les cliniciens à suivre leur hypothèse favorite et à essayer de "faire correspondre les caractéristiques" dans le cadre de cette hypothèse (Maitland et al, 2005). Afin de contrôler ce biais, un processus plus robuste de raisonnement hypothético-déductif, dans lequel de multiples hypothèses sont testées, est recommandé. Ce dernier dépend de la capacité des cliniciens à interpréter les résultats subjectifs et physiques et dépendra fortement de leur base de connaissances (Ryder, 2018). En écoutant et en adoptant ainsi des compétences de raisonnement narratif, le clinicien essaie de comprendre l'histoire du patient (Edwards et al, 2006) et intègre les pensées et les croyances du patient (Cooper et al 2008). Les informations données par le patient doivent être reconnues comme pertinentes et interprétées par le thérapeute. Ce processus dépend fortement de la base de connaissances du thérapeute. Un raisonnement clinique sain nécessite la métacognition et la réflexion critique, qui sont toutes deux importantes pour reconnaître les limites des connaissances (Jones, 2013). Si le clinicien pense qu'il manque des informations, il peut obtenir des éclaircissements sur l'exhaustivité des informations en utilisant des " questions de dépistage " pour d'autres types de symptômes.
Les cours de l'AMTI préconisent l'utilisation consciente du raisonnement clinique dès le premier moment où le patient nous consulte, en passant par l'examen physique, le traitement et la gestion globale jusqu'à la toute dernière rencontre. La réévaluation et la réflexion sont essentielles dans ce processus et sont particulièrement importantes lorsque les "caractéristiques ne correspondent pas" et que les hypothèses doivent être ajustées. Certains patients présentent des conditions qui semblent s'inscrire dans un schéma direct, mais en fin de compte, afin de promouvoir réellement la guérison et de résoudre le problème du patient, le clinicien et le patient doivent enquêter, examiner et réfléchir davantage pour trouver la cause du problème du patient. En particulier dans les domaines où la plupart des physiothérapeutes musculo-squelettiques (MSK PT) peuvent avoir des points aveugles dans leur connaissance et leur compréhension des mécanismes et des connexions sous-jacents.
Point aveugle : le plancher pelvien
Certains patients m'ont fait prendre conscience de mon angle mort et de la nécessité d'élargir mes connaissances et mes compétences pour reconnaître la cause des symptômes persistants autour du bassin. J'aimerais partager certaines de leurs histoires.
Exemple de patient 1 :
Une jeune mère et spécialiste en informatique, a présenté le diagnostic : "Tendinopathie de l'ischio-jambier proximal". Ilroblème principal : douleur aux fesses pendant travaillant assis à son bureau.
La patiente est venue nous voir après près d'un an d'échec de son traitement de rééducation en traitant le tendon localement et en appliquant elle-même le rouleau noir et les étirements. Il s'est avéré qu'elle souffrait également d'incontinence lors du jogging depuis la naissance de son deuxième enfant, il y a 3 ans. Elle aimait aller courir et avait commencé à le faire juste après l'accouchement pour se remettre en forme. Elle était très frustrée par le fait que, quels que soient ses efforts (exercices de base Pilates tous les jours et groupe de Cross-fit 3x par semaine), elle ne parvenait pas à retrouver son ancien niveau de forme. Ce n'est qu'après avoir consulté un spécialiste de la santé pelvienne qu'elle a pu courir sans problème. Elle a progressivement retrouvé son équilibre musculaire (y compris la relaxation de son tronc) et n'a plus de symptômes en position assise.
![]() Que dit la littérature ? Les exercices de CrossFit, qui impliquent des sauts, sont souvent liés à l'incontinence urinaire. Il est possible qu'une pression intra-abdominale élevée et des forces de réaction sur les organes pelviens soient impliquées dans ces activités à fort impact. Il est recommandé aux athlètes d'intégrer le renforcement du plancher pelvien dans leur programme d'entraînement. Les entraîneurs doivent sélectionner soigneusement les exercices pour éviter toute surcharge (Dominguez-Antuna et al, 2022).
Que dit la littérature ? Les exercices de CrossFit, qui impliquent des sauts, sont souvent liés à l'incontinence urinaire. Il est possible qu'une pression intra-abdominale élevée et des forces de réaction sur les organes pelviens soient impliquées dans ces activités à fort impact. Il est recommandé aux athlètes d'intégrer le renforcement du plancher pelvien dans leur programme d'entraînement. Les entraîneurs doivent sélectionner soigneusement les exercices pour éviter toute surcharge (Dominguez-Antuna et al, 2022).
Exemple de patient 2 :
A Patient de sexe masculin souffrant de douleurs de la ceinture pelvienne et de parästhésie dues à une consommation excessive d'alcool.  a développé une neuropathie des branches superficielles du nerf pudendal. Comme le patient souffrait également de dysfonctionnement sexuel, il a été orienté vers un PT en santé pelvienne.
a développé une neuropathie des branches superficielles du nerf pudendal. Comme le patient souffrait également de dysfonctionnement sexuel, il a été orienté vers un PT en santé pelvienne.
![]() Que dit la littérature ? Dans une revue sur le sujet, Chiaramonte et al (2021), ont constaté que tant les débutants que les cyclistes expérimentés peuvent développer des problèmes de nerfs pudendaux. La conception de la bicyclette, la posture ainsi que la conception du siège semblent jouer un rôle. La position debout sur les pédales, le repos et le passage à une vitesse supérieure ont été recommandés comme gestion. En outre, la neuropathie pudendale est décrite comme une "cause méconnue de douleur pelvienne qui peut être difficile à diagnostiquer et à traiter", bien qu'elle soit souvent associée au cyclisme, la pratique d'exercices d'accroupissement peut également en être la cause (Kasitinon et al, 2021).
Que dit la littérature ? Dans une revue sur le sujet, Chiaramonte et al (2021), ont constaté que tant les débutants que les cyclistes expérimentés peuvent développer des problèmes de nerfs pudendaux. La conception de la bicyclette, la posture ainsi que la conception du siège semblent jouer un rôle. La position debout sur les pédales, le repos et le passage à une vitesse supérieure ont été recommandés comme gestion. En outre, la neuropathie pudendale est décrite comme une "cause méconnue de douleur pelvienne qui peut être difficile à diagnostiquer et à traiter", bien qu'elle soit souvent associée au cyclisme, la pratique d'exercices d'accroupissement peut également en être la cause (Kasitinon et al, 2021).
Exemple de patient 3 :
Une patiente âgée obèse souffrant de lombalgies, de douleurs de la ceinture pelvienne et de la hanche gauche, qui présentait également un dysfonctionnement du plancher pelvien et une diverticulite comme comorbidités. Cette patiente avait des problèmes d'incontinence depuis qu'elle avait eu son premier enfant, il y a 50 ans ! Elle m'a dit qu'elle pensait qu'il était normal d'avoir ce genre de problèmes après l'accouchement...
Douleurs du plancher pelvien et douleurs lombopelviennes
La littérature récente montre qu'il existe une corrélation étroite entre le dysfonctionnement du plancher pelvien et les douleurs lombopelviennes. Le complexe du plancher pelvien est impliqué dans de nombreuses fonctions en dehors de son rôle biomécanique dans la stabilité, le contrôle et le transfert de force de la ceinture pelvienne (Pool-Goudzwaard, 2020). Le dysfonctionnement du plancher pelvien est parfois appelé " une épidémie silencieuse ", qui est " sous-reconnue et insuffisamment prise en charge " (Frawley, 2019).
Dysfonctionnement du plancher pelvien 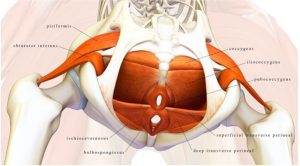 est un terme générique désignant toute anomalie ou déficience du plancher pelvien et des systèmes qui y sont associés. Cela inclut les muscles du plancher pelvien, les organes pelviens, les systèmes urogénital et colorectal. La douleur dans la région du plancher pelvien peut également provenir d'une pathologie viscérale et il existe des pathologies graves qui se produisent dans la région pelvienne et qui peuvent passer inaperçues.
est un terme générique désignant toute anomalie ou déficience du plancher pelvien et des systèmes qui y sont associés. Cela inclut les muscles du plancher pelvien, les organes pelviens, les systèmes urogénital et colorectal. La douleur dans la région du plancher pelvien peut également provenir d'une pathologie viscérale et il existe des pathologies graves qui se produisent dans la région pelvienne et qui peuvent passer inaperçues.
Le fait de ne pas tenir compte du plancher pelvien en tant qu'élément important de la douleur de la ceinture pelvienne peut entraîner une prise en charge inappropriée du patient et retarder inutilement l'amélioration de son état (Röscher, 2021). Très souvent, les patients présentant des douleurs lombopelviennes ou de la ceinture pelvienne sont associés à un dysfonctionnement des muscles du plancher pelvien. Dans une étude de Dufour et al (2018), dans une cohorte de 85 femmes présentant des douleurs lombopelviennes, 95,3% présentaient un degré de dysfonctionnement pelvien.
Physiothérapeutes musculo-squelettiques (MSK) avoir idéalement une compréhension de base du plancher pelvien et des dysfonctionnements qui y sont associés, afin d'être en mesure de dépister ces patients et, le cas échéant, de les orienter vers un professionnel du plancher pelvien (De Ruijter & Röscher, sous presse).
Rôles et limites des compétences d'un thérapeute MSK par rapport au plancher pelvien.
Au cours de l'examen de contrôle, chaque thérapeute spécialisé dans les troubles musculo-squelettiques doit être prêt à poser des questions spécifiques sur une éventuelle dysfonction du plancher pelvien comme cause ou comme facteur contribuant aux symptômes du patient. En général, les patients ne partagent pas automatiquement les informations sur la dysfonction du plancher pelvien dans un contexte musculo-squelettique. Par conséquent, il peut être difficile pour le thérapeute de poser des questions spécifiques sur la dysfonction du plancher pelvien. Il se peut que le thérapeute musculo-squelettique se sente gêné ou perçoive que le patient pourrait être gêné par ce type de questions. Même dans un cadre médical, Ben Charif et al (2016), ont constaté que seulement 20% des patients atteints de cancer ont parlé à leur médecin de leur dysfonctionnement sexuel. Afin de faciliter cette situation, fournir un questionnaire au patient pourrait être un moyen d'obtenir des informations d'une manière non menaçante. Dans le cas où le questionnaire indique une implication du plancher pelvien, il sera plus facile pour le thérapeute d'utiliser cette information et de l'utiliser pour faire le pont afin d'obtenir des précisions supplémentaires.
Sur la base de l'Australian Pelvic Floor Questionnaire et de Frawley et al (2021), Röscher (2022) suggère d'utiliser la question suivante pour obtenir le consentement pour poser des questions relatives au plancher pelvien: "Certaines personnes souffrant de douleurs pelviennes ont également des problèmes avec leur plancher pelvien. Puis-je vous poser des questions sur vos fonctions vésicale, intestinale et sexuelle ?"
- Pour demander spécifiquement dysfonctionnement de la vessievous pourriez demander : "Est-ce que vous avez des fuites d'urine en toussant, en éternuant, en riant ou en faisant de l'exercice ?" "Est-ce que l'urine fuit lorsque vous vous précipitez ou que vous n'arrivez pas à temps pour aller aux toilettes ?".
- Questions à poser sur dysfonctionnement des intestins: "Vous sentez-vous constipé ou avez-vous du mal à vider vos intestins ?" "Avez-vous parfois des fuites de selles ?"
- Enfin, pour demander symptômes moteurs des muscles du plancher pelvien: "Votre plancher pelvien vous semble-t-il lâche, laxiste, béant, affaissé, ouvert, faible, bombé, lourd, plein ou difficile à détendre, serré, tendu, étroit ou resserré ?". (Röscher, 2021).
Si le PT MSK émet l'hypothèse que le plancher pelvien pourrait être impliqué dans le problème principal du patient, il faut l'adresser à un spécialiste de la santé pelvienne. La tâche du spécialiste de la santé pelvienne implique une évaluation échographique spécifique, une observation externe et un examen vaginal ou rectal interne. Les dysfonctions du plancher pelvien peuvent être divisées en plusieurs troubles spécifiques et la prise en charge peut varier en conséquence (Frawley et al, 2021).
En l'absence de formation et d'expérience spécifiques en matière d'évaluation et de traitement des dysfonctionnements du plancher pelvien, il est déconseillé de commencer à faire des exercices pelviens avec ces patients, car cela pourrait aggraver leur état. Il est fortement recommandé de commencer à constituer un réseau de collègues compétents ayant de l'expérience dans ce domaine, de collaborer et d'élargir votre horizon professionnel en posant les questions appropriées pour tenter de découvrir la "cause de la cause" des signes et symptômes du patient.
Références :
Ben Charif, A., Bouhnik, A-D., Courbière, B., Rey, D., Préau, M., Bendiane, M-K., Peretti-Watel P., et Mancini, J. (2016). Problèmes de santé sexuelle chez les survivants français du cancer 2 ans après le diagnostic - Enquête nationale VICAN. Journal of Cancer Survivorship 10, no. 3 (juin 2016) : 600-609. https://doi.org/10.1007/s11764-015-0506-3.
Chiaramonte, R., Pavone, P., et Vecchio, M. (2021). Diagnostic, réhabilitation et stratégies préventives de la neuropathie pudendale chez les cyclistes, une revue systématique. Journal de la morphologie fonctionnelle et de la kinésiologie 6, no. 2 : 42. https://doi.org/10.3390/jfmk6020042.
Cooper et al (2008) in : Petty, N. J., & Ryder, D. (Eds.). (2017). Musculoskeletal Examination and Assessment E-Book : Un manuel pour les thérapeutes. Elsevier Health Sciences.
De Ruijter, R., Röscher, M. in : Hengeveld, E. & Bucher-Dollenz, G. (sous presse). Le concept Maitland de la physiothérapie NMSK - Évaluation et gestion des fonctions du mouvement NMSK. Vol 2 : Clinical Application. 6ème édition. Chapitre : Ceinture pelvienne, examen et prise en charge. Elsevier, Oxford.
Dominguez-Antuña, E., Diz, J. C., Suárez-Iglesias, D. et Ayán C. (2022). Prévalence de l'incontinence urinaire chez les athlètes féminines de CrossFit : A Systematic Review with Meta-Analysis. Journal international d'urogynécologie, 30 mai. https://doi.org/10.1007/s00192-022-05244-z.
Dufour, S. (2018). Association entre les douleurs lombopelviennes et les dysfonctionnements du plancher pelvien chez les femmes_ Une étude transversale. Science et pratique de l'appareil locomoteur, 7.
Edwards, I., Jones, M., et Hillier, S. (2006). L'interprétation de l'expérience et sa relation avec le mouvement du corps : A Clinical Reasoning Perspective. Thérapie manuelle 11, no. 1 : 2-10. https://doi.org/10.1016/j.math.2005.10.002.
Feltowich, P.J. et Barrows, H.S., (1984). Issues of generality in medical problems solving. Dans : Petty, N. J., & Ryder, D. (Eds.). (2017). Musculoskeletal Examination and Assessment E-Book : Un manuel pour les thérapeutes. Elsevier Health Sciences.
Frawley, H. C., Neumann P., et Delany, C. (2019). Un argument en faveur de la formation basée sur les compétences dans la pratique de la physiothérapie du plancher pelvien. Théorie et pratique de la physiothérapie 35, no. 12 : 1117-30. https://doi.org/10.1080/09593985.2018.1470706.
Frawley, H., Shelly, B., Morin, M., Bernard M., Bø, K., Digesu, G.A., Dickinson, T. Un rapport de l'International Continence Society (ICS) sur la terminologie de l'évaluation des muscles du plancher pelvien. Neurourologie et Urodynamique 40, no. 5 (juin 2021) : 1217-60. https://doi.org/10.1002/nau.24658.
Hengeveld, E. & Banks, K. (Eds.). (2013). Manipulation vertébrale de Maitland : Gestion des troubles neuromusculosquelettiques - Volume 1 (Vol. 1). Elsevier Health Sciences.
Jones, M. dans : Hengeveld, E. & Banks, K. (Eds.). (2013). Manipulation vertébrale de Maitland : Gestion des troubles neuromusculosquelettiques - Volume 1 (Vol. 1). Elsevier Health Sciences.
Kasitinon, D., Kelly, B., Price, T. L., Chhabra, A., & Scott, K. M. (2021). Blessures des nerfs pudendaux dans les sports et l'exercice : une série de cas de neuropathies pudendales dues aux squats. Journal de la physiothérapie pour la santé des femmes, 45(1), 3-9.
Maitland, G. D., Hengeveld, E., Banks, K., & English, K. (2005). La manipulation vertébrale de Maitland: Elsevier Butterworth.
Pool-Goudzwaard, A., Beales, D. et Bussey, M. (2020). Introduction au numéro spécial sur les douleurs pelviennes. Science et pratique de l'appareil locomoteur.48 102168. https://doi.org/10.1016/j.msksp.2020.102168.
Röscher M. (2021). Diapositives du cours "The Functional Pelvis" (cours en ligne). www.physioskills.com.au
Ryder D. Dans : Petty, N. J., & Ryder, D. (Eds.). (2017). Musculoskeletal Examination and Assessment E-Book : Un manuel pour les thérapeutes. Elsevier Health Sciences.








Commentaires